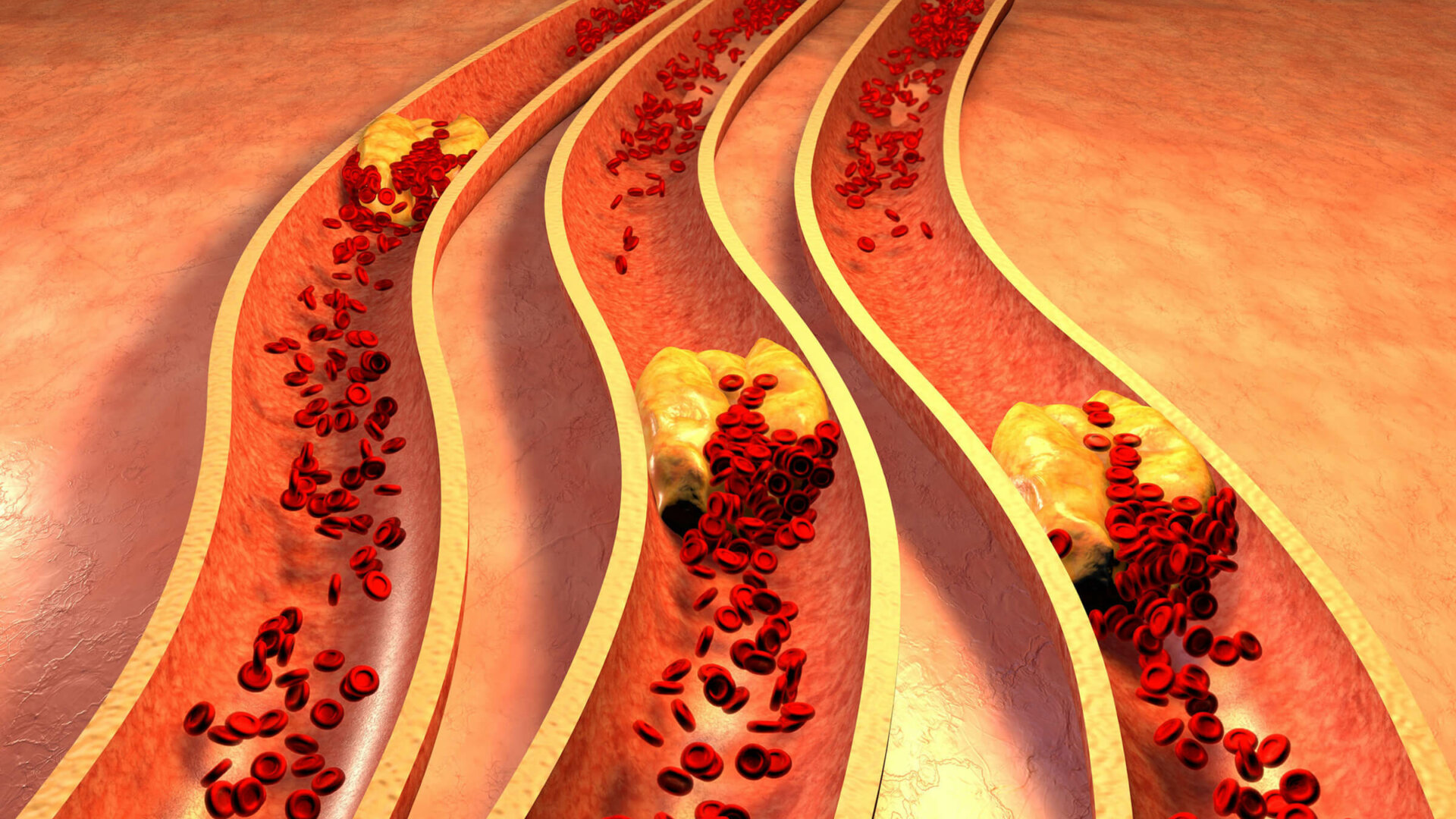
If you’ve been to your doctor’s office, chances are you’ve had your blood drawn. This is standard practice in the medical field as it provides data for the practitioner to assess the current states of lab data on their respective patient. As the saying goes, you can’t manage what you don’t measure.
One of the most common biomarkers measured is cholesterol. This is often looked at to assess potential risk for serious heart problems or to help manage someone’s cholesterol levels that have a personal or family history of hyperlipidemia (high cholesterol) or are taking cholesterol lowering medications. In 2011-2012, the United States had approximately 78 million adult cases of medication warranting levels of LDL-Cholesterol (low-density lipoprotein), also known as “bad cholesterol”. [1]
In this article, we will go into detail about cholesterol, different cholesterol particles, what can affect our levels, and what we can possibly do to help improve levels that need improving. Please note: this article is not meant to diagnose or treat a medical condition. It is meant to raise awareness and help educate the reader.
What is Cholesterol?
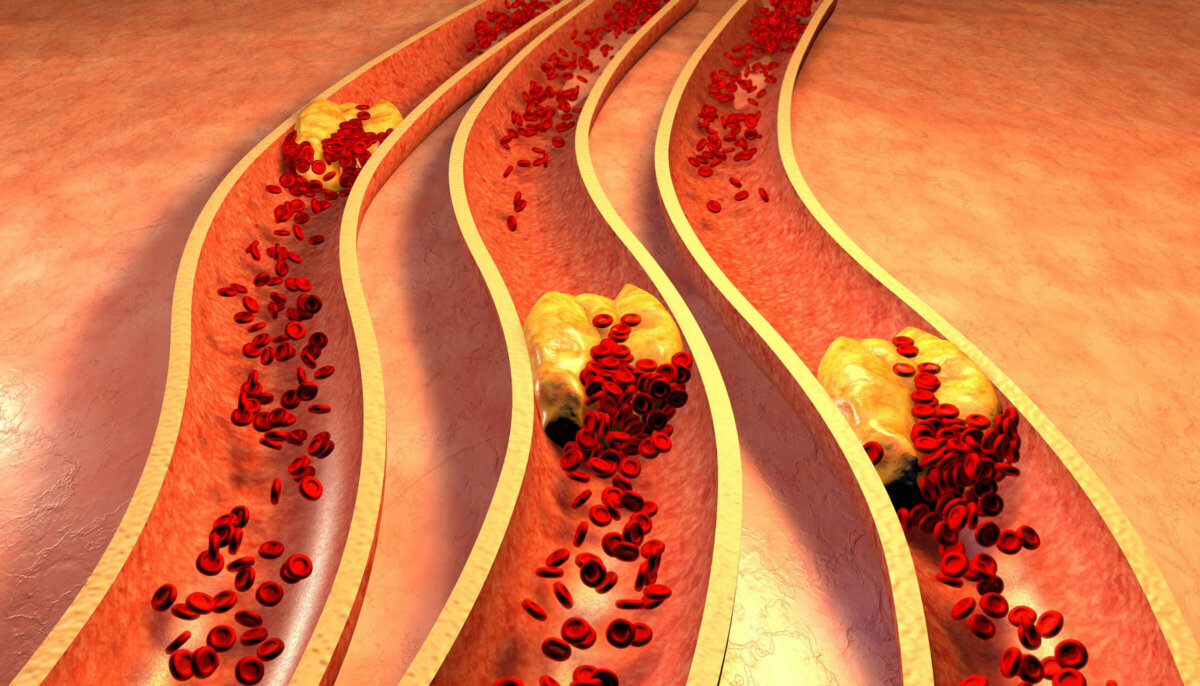
Cholesterol is naturally found in our bodies, and we can thank our liver for that. Our body produces the cholesterol we need. Not all cholesterol is bad. We technically need cholesterol for our cells and hormones to function properly. We also get cholesterol from animal foods in our diet. NOTE* Do not be fooled by marketing from food companies; if the label reads cholesterol-free, it is because it does not come from an animal.
Cholesterol travels through our bodies in lipoproteins, each with different functions. Lipoproteins are molecules made up of fat and protein. These lipoproteins take cholesterol to our liver to be recycled or to our arteries to eventually get back in our blood and then recycled again, and so on. It is also important to note that there are different types of particles of good and bad cholesterols. See the different breakdowns below.
The breakdown of cholesterol types are as follows:
- HDL (High Density Lipoprotein)- Often known as the “good cholesterol.” Moves cholesterol from arteries to the liver, almost like a Drano® type of lipoprotein. This cholesterol makes up ~30% [2].
- LDL (Low Density Lipoprotein)- Referred to as the “bad cholesterol.” This is the cholesterol that causes damage/hardening to/of arteries and it makes up for ~60% of total cholesterol [2].
- VLDL (Very Low Density Lipoprotein- A type of the “bad cholesterol.” This cholesterol is a type of precursor to LDL and makes up ~10% of total cholesterol [2].
- Triglycerides- a form of fat stored in the blood which effects cholesterol readings.
- Remnant lipoprotein- a culprit in the causation of platelets aggregating and being a high cause of arterial damage [3].*
- Apo A-I- associated with the cardio-protective HDLs. Plays a crucial role in transporting cholesterol from tissues (arteries) to the liver [4].*
- Apo B- associated with the plaque causing LDLs. Important in transportation of lipids to arteries [4]*
- Lipoprotein(a) a.k.a. Lp(a)- a highly atherogenic (plaque causing) lipoprotein that poses a potential threat as a lone factor, meaning regardless of LDL levels, Lp(a) poses a threat. This is mostly secondary due to genes or familial history [5].*
Note* Not measured on common lab panels; typically measure by specialty testing/labs*
As one can see, there are many factors to consider when analyzing a lipid profile. It is important to mention that some of these tests are not commonly ordered by physicians or nurse practitioners. To have these values measured, one would typically have to use a specialty lab, but always consult with your healthcare provider as they are responsible for ordering these tests.
A Genetic marker not very well known: ApoE
Apolipoprotein E a.k.a. ApoE is a genetically passed-down lipoprotein. ApoE is a lipoprotein responsible for distributing lipids throughout different cells in the body and is also referred to as the “Alzheimer’s Gene [6] .” The functionality of this gene is dependent on the potential disequilibrium or structural difference in the 19th human chromosome [6]. There are different variations of this genetic expression. E3 is known as the most common, where E2 and E4 are considered not normal or defective and raise potential risk factors in lipid metabolism (cholesterol issues) [7]. The gene expression is read on a report as E3/E3, one from each parent. The different possible variations are:
- E2/E2
- E2/E3
- E2/E4
- E3/E3
- E3/E4
- E4/E4
These genes may even impact how much animal protein we consume and how intense our exercise should be performed. When genetic testing is done, remember it is not a diagnosis of an illness, only the presence of a genetic mutation or structural deformity. Yes, it raises awareness of potential risk of an illness or illnesses, but lifestyle contributes a great deal to what happens.
What can we do about high cholesterol and/or not-so-great genes?

Lifestyle has the power to reverse disease (i.e. losing weight can help decrease high blood pressure), manage illness (i.e. use little to no insulin in type 2 diabetes), and keep genetics in check (i.e. someone having normal cholesterol levels despite family history). Below are several behavioral strategies that one can incorporate to help manage cholesterol levels (always consult with your physician before attempting to make a change/start something new such as taking niacin [see below]):
- Exercise regularly [8]
- Eat a diet lower in saturated fat(7% or less calories from saturated fats) and higher in monounsaturated fats [8]
- Incorporate more omega-3 polyunsaturated fats derived from marine animals (i.e. salmon) [8]
- Alcohol consumption may help increase HDL, but also has potential to increase triglyceride levels [8]. Avoiding excess alcohol may be best (equivalent of 1 glass of wine for women, 2 glasses for men are standard suggestions)
- Taking niacin may help with decreasing LDL cholesterol as well as triglycerides and may increase HDL [9]
- Increasing fiber consumption, 20-30g daily [8],[9]
- Lastly, working with a registered dietitian for medical nutrition therapy counseling [10]
Take Home Message
Cholesterol can be the cause of other issues such as heart attack or stroke, but leading an active and healthy lifestyle can help. Being active and eating leaner proteins, higher fiber foods as well as healthy fats all help keep cholesterol under control. Talk with your physician to discuss what can be done or measured to help ensure optimal health for yourself. Remember, genetics play an important role in our health, but our lifestyle has the potential to overrule those genes.
References
- https://www.cdc.gov/cholesterol/facts.htm
- https://www.health.harvard.edu/heart-health/making-sense-of-cholesterol-tests
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3259494/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3972591/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3295201/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5973862/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4253862/
- https://www.ncbi.nlm.nih.gov/books/NBK218744/
- https://www.nhlbi.nih.gov/files/docs/guidelines/atp3xsum.pdf
- https://www.lipidjournal.com/article/S1933-2874(18)30274-5/fulltext?dgcid=raven_jbs_etoc_email